
Forschung Pankreaszentrum
Welcome to the Website of the Pancreatic Neuropathy and Pain Research Group. We belong to the Department of Surgery at the Technical University of Munich
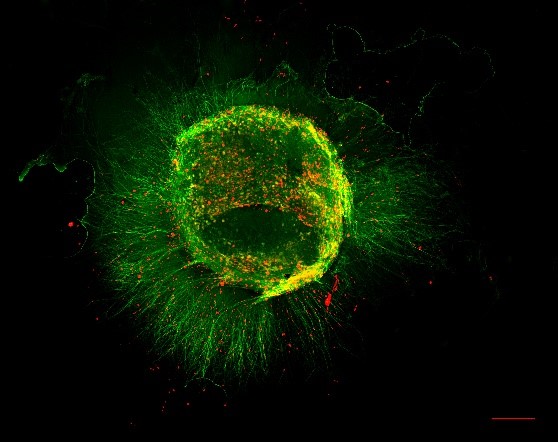 As clinician-scientists, we perform both basic science and clinical research for elucidating the clinically relevant aspects of human pancreatic cancer and chronic pancreatitis. Our research integrates molecular biology with in-depth characterization of human pancreatic tissue, advanced 3D heterotypic cultures models, live cell imaging, genetically engineered mouse models (GEMMs) of pancreatic cancer, and mouse models of acute and chronic pancreatitis. We are part of the Collaborative Research Centre 1321 (Modelling and Targeting of Pancreatic Cancer), of the DKTK (German Cancer Consortium) Munich site, and of the Pancreatic Cancer Alliance Munich (PCAM).
As clinician-scientists, we perform both basic science and clinical research for elucidating the clinically relevant aspects of human pancreatic cancer and chronic pancreatitis. Our research integrates molecular biology with in-depth characterization of human pancreatic tissue, advanced 3D heterotypic cultures models, live cell imaging, genetically engineered mouse models (GEMMs) of pancreatic cancer, and mouse models of acute and chronic pancreatitis. We are part of the Collaborative Research Centre 1321 (Modelling and Targeting of Pancreatic Cancer), of the DKTK (German Cancer Consortium) Munich site, and of the Pancreatic Cancer Alliance Munich (PCAM).
 Importantly, we derive our research questions and objectives directly from the human tissue and human disease, and aim at developing in vitro and in vivo models that best mimic the human conditions. Our research group is an international team of biologists and clinicians with the aim to uncover selected disease mechanisms in pancreatic disease with the ultimate goal of developing novel therapy strategies.
Importantly, we derive our research questions and objectives directly from the human tissue and human disease, and aim at developing in vitro and in vivo models that best mimic the human conditions. Our research group is an international team of biologists and clinicians with the aim to uncover selected disease mechanisms in pancreatic disease with the ultimate goal of developing novel therapy strategies.
The main three lines of investigation in our laboratory are as follows:
1) Mechanisms of neural invasion and neuropathy in human pancreatic Cancer
Co-Investigators: Istvanffy, Wang
Neural invasion is one of hallmarks of human pancreatic cancer and pancreatic neuropathy, and it drastically worsens the prognosis of patients due to early recurrence. We developed novel research tools for simulating neural invasion in 3D culture and, together with our collaboration partners, characterized novel GEMMs of pancreatic cancer that exhibit human-like neural invasion. We currently focus on the role of Schwann cells, stromal cells (i.e. cancer-associate fibroblasts), mesenchymal stem cells, and especially immune cells as potential inducers of neural invasion.
2) Tumor immune profile in locally advanced and resectable pancreatic Cancer
Co-Investigators: Istvanffy, Safak, Mota-Reyes
Neoadjuvant therapy has remarkably improved the prognosis of patients with locally advanced pancreatic cancer, who can in ca. 60% of cases become candidates for surgical resection after tumor downsizing. We are applying novel mouse models that allow the application of neoadjuvant therapy similar to the clinical setting, and analyse the immune profile of neoadjuvantly treated versus primary resected pancreatic cancer in simultaneous comparison with human specimens.
3) Pain mechanisms in pancreatitis and pancreatic Cancer
Co-Investigators: Schorn, Safak
By far, the most unpleasant symptom of pancreatitis and pancreatic cancer is severe abdominal and/or back pain. We have recently identified the molecular, neuro-immune mediators of pain in both diseases and are currently performing pre-clinical analgesic trials for more effective pain treatment in pancreatic diseases.
Our research is funded by Deutsche Forschungsgemeinschaft (DE2428/3-1, DE2428/3-2, DE2428/6-1, SFB/CRC 1321 subproject P07), Deutsche Krebshilfe (Nr. 70112897), Wilhelm-Sander Stiftung (2015.160.1, 2019.091.1), Stiftung Chirurgie at TUM, intramural funds of the TUM, and industry.
We thank you for your interest in our research.
 Ihsan Ekin Demir, MD, PhD
Ihsan Ekin Demir, MD, PhD
Principal Investigator
Pancreatic Neuropathy & Pain Research Group



















 erhält Young Investigator Grant 2023 der IAP und der APA Foundation für Forschung
erhält Young Investigator Grant 2023 der IAP und der APA Foundation für Forschung 














